Grey's Anatomy TV Series Medical Review (S2E24)
- Mar 29
- 9 min read

Welcome to the pit, folks. Grab your coffee—preferably a cappuccino if you’re trying to impress Burke—and let’s talk about a shift that defines "Damage Control". We had a multi-car pileup that flooded the ER with everything from minor lacerations to catastrophic multisystem trauma. We saw a pregnant patient whose initial stability was a deceptive mask of adrenaline, her husband with a shattered leg, and the confused driver who caused the mess. Meanwhile, in the ORs and wards, we dealt with a virtuoso whose heart was literally out of sync with his art, a mother of six at her absolute breaking point, and a high-powered attorney who was actually begging for a seizure just so she could get back to the courtroom. It’s the kind of day where the "Triangle of Death" isn’t just a textbook concept; it’s the monster under the bed.
Let’s go to rounds.

Catastrophic Internal Injuries
Diagnosis
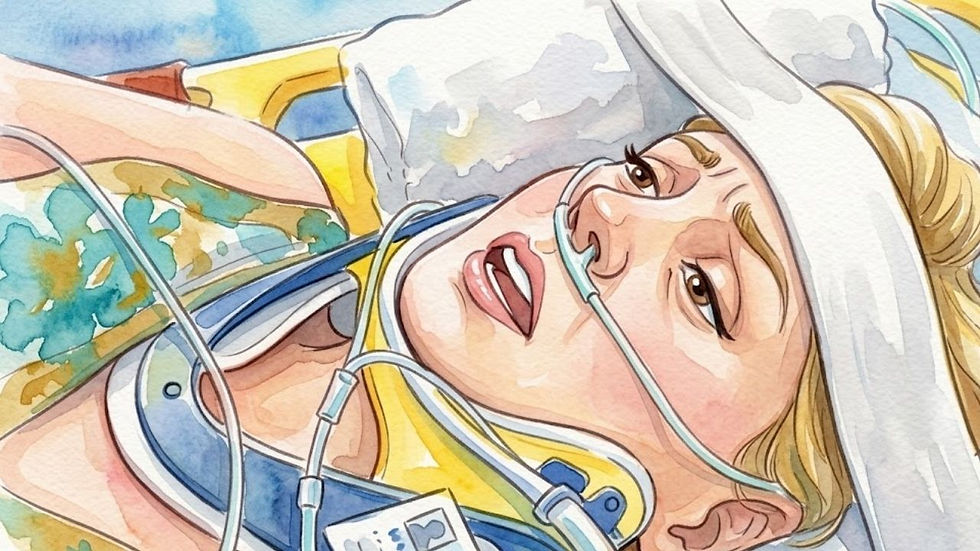
Multisystem Trauma with Hemorrhagic Shock.
Definition
Severe, life-threatening injuries to multiple organ systems are typically caused by high-energy blunt force trauma. This leads to a "Triangle of Death"—a lethal combination of acidosis, coagulopathy, and hypothermia—where the body’s physiological reserves are exhausted. Prognosis is guarded and depends on rapid surgical intervention and "damage control" stabilization.
Patient
Melanie Reynolds.
Case Summary
A 22-year-old pregnant woman was brought in after a car accident. Her body initially masked the severity of her injuries with adrenaline. Once she relaxed, she crashed and was rushed to surgery for a splenectomy and lung resection. The team attempted "damage control" by packing her and moving her to the ICU to stabilize before returning to the OR, but she unfortunately died on the table.
Care Team
Derek Shepherd, Preston Burke, Addison Forbes Montgomery, Richard Webber, Miranda Bailey, Cristina Yang, and Alex Karev.
Treatment
Splenectomy, lung resection, packing for damage control, and posthumous delivery of her infant.
What they did wrong
Doctors noted that her shock concealed the extent of her catastrophic injuries. In modern trauma care, clinicians do not wait for "shock to wear off" to find injuries; they use immediate FAST exams (Focused Assessment with Sonography for Trauma) and CT scans to identify internal bleeding regardless of a patient's adrenaline levels. Additionally, despite their efforts, she died on the table, and her baby was delivered posthumously—a high-risk scenario that often indicates a delay in stabilizing the mother or performing a perimortem cesarean section.
What they did right
They correctly identified the "triangle of death" (acidosis, hypothermia, and coagulopathy) during surgery. Their decision to perform damage control surgery—packing the patient and moving her to the ICU to stabilize before returning to surgery hours later—is the gold standard for treating major trauma today.

Pacemaker Malfunction
(Rhythm Displacement)
Diagnosis
Pacemaker-Induced Dysrhythmia or Sub-optimal Pacing Parameters.
Definition
A condition where an implanted cardiac pacemaker fails to maintain an appropriate heart rhythm for the patient's specific physiological needs, or where the electronic pacing interferes with the patient's natural hemodynamic flow. Manifestations include fatigue, palpitations, or, for a musician, a perceived loss of "rhythm." Prognosis is excellent with recalibration or lead revision.
Patient
Eugene Foote.
Case Summary
A world-renowned violinist who felt his pacemaker had changed his "rhythm," making it impossible for him to play. Despite Burke’s attempts to adjust the settings, Foote insisted on a risky surgery to remove scar tissue around the device to regain his musical "soul," knowing the surgery could be fatal.
Care Team
Preston Burke and George O’Malley.
Treatment
Multiple pacemaker adjustments followed by a high-risk surgical revision of the device and surrounding fibrotic tissue.
What they did wrong
The patient felt his pacemaker was interfering with his "artistic rhythm" . In modern medicine, it is rare to perform a high-risk surgery to remove scar tissue around a functional, life-saving device simply for "artistic feel" without clear physiological evidence of malfunction.
What they did right
Dr. Burke initially attempted to adjust the pacemaker's settings non-invasively to accommodate the patient's lifestyle before resorting to surgery.
Grand Mal Seizures (Intractable Epilepsy)
Diagnosis
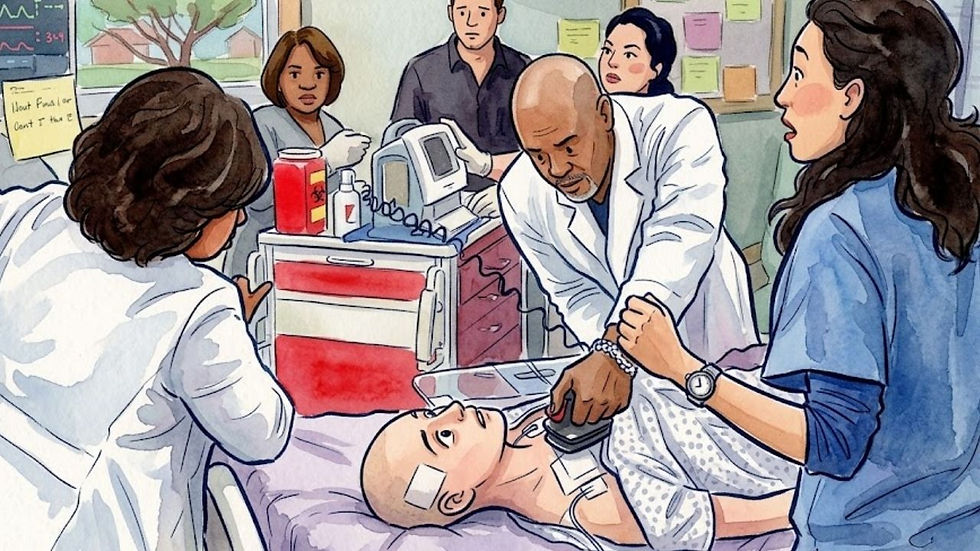
Refractory Focal Epilepsy.
Definition
A chronic neurological disorder characterized by recurrent, unprovoked seizures that do not respond to standard anticonvulsant medications. Manifestations include loss of consciousness and muscle contractions. Surgical intervention requires "brain mapping" to locate the seizure focus. Prognosis varies based on the success of the focal resection.
Patient
Mrs. Graber.
Case Summary
A divorce lawyer was admitted for brain mapping to locate the source of her seizures for surgical removal. She grew frustrated after three days without a seizure and attempted to "induce" one using sleep deprivation, caffeine, and even a high-level video game. After witnessing a heated argument between interns, she finally suffered a seizure, allowing the team to map the area for surgery. She ultimately decided against the craniotomy, choosing to change her stressful lifestyle instead.
Care Team
Derek Shepherd and Izzie Stevens.
Treatment
Brain mapping (EEG monitoring), provoked seizure through environmental stressors, and proposed craniotomy (declined by patient).
What they did wrong
The interns used highly unconventional and potentially dangerous methods to induce a seizure, including forcing the patient to consume excessive caffeine and sugar (donuts) and play video games to the point of exhaustion. Additionally, the doctors' personal bickering in front of the patient was unprofessional.
What they did right
The core goal—brain mapping—was correct. Using sleep deprivation to lower the seizure threshold is a standard clinical practice in an Epilepsy Monitoring Unit (EMU) to locate the seizure focus before surgical resection.

End-Stage Heart Failure
Diagnosis
Congestive Heart Failure (CHF).
Definition
A chronic, progressive condition where the heart muscle is unable to pump enough blood to meet the body's needs for blood and oxygen. Manifestations include edema, fatigue, and shortness of breath. Prognosis is poor without a transplant or mechanical support.
Patient
Denny Duquette, Jr.
Case Summary
A long-term cardiac patient currently living on a Left Ventricular Assist Device (LVAD). He pushed himself too hard on his current machine and collapsed. He spent the episode lobbying for a portable LVAD to regain some semblance of a normal life and "stop urinating in a bag".
Care Team
Preston Burke, Miranda Bailey, Izzie Stevens, and Meredith Grey.
Treatment
Continuous LVAD support and transition to a portable LVAD unit.
What they did wrong
The most significant error was the lack of professional boundaries. Dr. Izzie Stevens became romantically involved with her patient, leading to biased medical advice. Furthermore, Denny collapsed after "pushing himself too far" on his LVAD, suggesting he was not being monitored closely enough or was not properly educated on the device's physical limitations.
What they did right
The medical team used an LVAD (Left Ventricular Assist Device) to keep him alive while waiting for a heart transplant. Transitioning him to a portable LVAD is the standard of care for patients who need "bridge-to-transplant" therapy, allowing them more mobility and a better quality of life.

Voluntary Sterilization via Tubal Ligation

Diagnosis
Multiparity-associated Exhaustion (and Surgical Sterilization Request).
Definition
While not a "disease," grand multiparity (having 5 or more births) can lead to significant physiological and psychological exhaustion. Tubal ligation is a permanent surgical procedure to prevent pregnancy by blocking the fallopian tubes. Prognosis for recovery is excellent.
Patient
Rose Ward.
Case Summary
A 38-week pregnant mother of six was admitted for a C-section. Desperate to stop having children due to extreme exhaustion and religious pressure from her husband, she requested a secret tubal ligation. Addison performed the procedure and covered it as a "surgical complication" involving "unexpected bleeding" and "damaged tubes" to protect the patient's domestic safety.
Care Team
Addison Forbes Montgomery and Alex Karev.
Treatment
Cesarean section and bilateral tubal ligation (documented as a surgical complication).
What they did wrong
This case involved a massive ethical and legal breach. To satisfy Rose's request to have her tubes tied without her husband's knowledge, Dr. Addison Montgomery and the interns performed the procedure and then lied, calling it a "complication" from "unexpected bleeding" that "damaged" the tubes. This is considered medical malpractice and insurance fraud, as they intentionally falsified surgical records to hide a requested procedure.
What they did right
Dr. Addison correctly asserted that Rose is an adult and her husband is not her "legal guardian," meaning she has the right to make her own reproductive choices without his consent. This prioritizes patient autonomy, which is a central pillar of modern medicine.

Patella Fracture
Diagnosis
Displaced Patella Fracture.
Definition
A break in the kneecap, usually caused by a direct blow or a sudden forceful contraction of the quadriceps. Manifestations include localized pain, swelling, and inability to extend the knee. Prognosis is generally good with surgical fixation.
Patient
Noah Reynolds.
Case Summary
A 25-year-old man was brought to the ER after a car accident. He presented with significant right knee pain.
Care Team
Callie Torres and Izzie Stevens.
Treatment
Surgical reduction and fixation.

Traumatic Brain Injury & Wrist Fracture

Diagnosis
Closed Head Injury and Distal Radius Fracture.
Definition
A head injury where the skull remains intact but the brain is subjected to force, leading to confusion or altered consciousness. A broken wrist is a common orthopedic injury following trauma. Prognosis for both is typically good with monitoring and immobilization.
Patient
Marshall Stone.
Case Summary
The driver is responsible for the car accident. He presented to the ER confused and was found to have a closed head injury and a broken wrist.
Care Team
Derek Shepherd, Callie Torres, Meredith Grey, and George O’Malley.
Treatment
Reduction and splinting of the wrist; CT scan (which was clear) to monitor the head injury.

Neonatal Care / Posthumous Birth
Diagnosis
Neonatal Observation.
Definition
The clinical monitoring of a newborn, particularly one delivered under traumatic circumstances, to ensure respiratory and hemodynamic stability.
Patient
Baby Reynolds.
Case Summary
The baby was delivered via emergency C-section just as the mother, Melanie, passed away.
Care Team
Addison Montgomery-Shepherd and Alex Karev.
Treatment
Immediate transfer to the Neonatal Intensive Care Unit (NICU) for specialized care.

Scalp Laceration

Diagnosis
Scalp Laceration.
Definition
A tear or cut in the skin of the scalp, which is highly vascular and prone to significant bleeding. Prognosis is excellent with proper cleaning and closure.
Patient
Jim Johnson.
Case Summary
A car accident victim was brought in with a bleeding scalp.
Care Team
Miranda Bailey and George O’Malley.
Treatment
Stitches, bandaging, and a clear CT scan before discharge.

Trauma Assessment (Negative)
Diagnosis
No acute injuries.
Definition
The clinical process of ruling out life-threatening injuries following a traumatic event.
Patient
Betty Johnson.
Case Summary
A car accident victim was examined in the ER.
Care Team
Alex Karev.
Treatment
Physical examination and CT scans (which were clear), followed by discharge.

Paraesophageal Hernia

Diagnosis
Paraesophageal (Type II) Hiatal Hernia.
Definition
A condition where a portion of the stomach protrudes through the diaphragm and sits alongside the esophagus. Unlike sliding hernias, these carry a risk of incarceration or strangulation. Prognosis is excellent following surgical repair.
Patient
Unnamed.
Case Summary
A patient is scheduled for a routine surgical repair.
Care Team
Cristina Yang.
Treatment
Surgery.

Ruptured Abdominal Aortic Aneurysm (AAA)
Diagnosis
Ruptured Abdominal Aortic Aneurysm.
Definition
A life-threatening emergency where the wall of the aorta weakens and bursts, leading to massive internal hemorrhage. Manifestations include sudden, severe abdominal or back pain and hypotension. Prognosis is poor without immediate vascular surgery.
Patient
Unnamed.
Case Summary
A high-intensity trauma case was mentioned by intern Marshall Stone.
Care Team
Marshall Stone (Scrubbed in).
Treatment
Emergency surgery.

Surgical Case (OB/GYN)
Diagnosis
Unknown.
Definition
N/A.
Patient
Unnamed.
Case Summary
A patient requiring immediate surgical intervention forced Addison to leave the Reynolds case.
Care Team
Addison Montgomery-Shepherd.
Treatment
Surgery.

🔖 Key Takeaways
🗝️ A mass-casualty crash highlights the importance of rapid trauma assessment, early imaging, and damage control surgery in preventing the “triangle of death.”
🗝️ The episode balances accurate medical practices—like LVAD therapy and brain mapping—with dramatized or unsafe methods, especially in seizure induction and surgical decision-making.
🗝️ Ethical dilemmas take center stage, from falsified surgical records in a secret tubal ligation to blurred doctor-patient boundaries in Denny’s case.
🗝️ Patient autonomy is strongly emphasized, particularly in reproductive rights and treatment refusal, even when it conflicts with medical or legal norms.
🗝️ The episode ultimately shows that in high-pressure medicine, outcomes depend not just on skill, but on timing, ethics, and emotional control.
Keywords: Grey's Anatomy S2E24







Comments